Reduce Costs, Increase Efficiency: The ROI of Implementing Telemedicine Systems for Large Hospitals

Telemedicine is the delivery of medical services via remote communication technologies, such as video calls, medical robots, and digital platforms. It allows doctors to diagnose and monitor patients without in-person visits. For large hospitals, investing in a Telemedicine system yields an average ROI of 150–300% within 3 years, reducing personnel costs by 20–35% and energy costs by 15–25%.
Table of Contents
What is Telemedicine, and Why Should Large Hospitals Care?
In an era where the Thai healthcare system faces pressure from rising costs, medical staff shortages, and an increasing volume of patients every year, Telemedicine has become the key that top hospital executives worldwide choose to transform cost management and service quality simultaneously.
The Telemedicine system is no longer just 'video calling with a doctor.' It now covers everything from Remote Patient Monitoring (RPM) systems and AI diagnostic platforms to autonomous mobile medical robots. This enables hospitals to provide more services with the same or fewer resources, perfectly meeting the requirements of being a Smart Hospital .
Types of Telemedicine Popular in Large Hospitals
Real-time video consultation, suitable for OPD and chronic patient monitoring.
Sending patient data, X-rays, or lab results in advance for doctors to diagnose later.
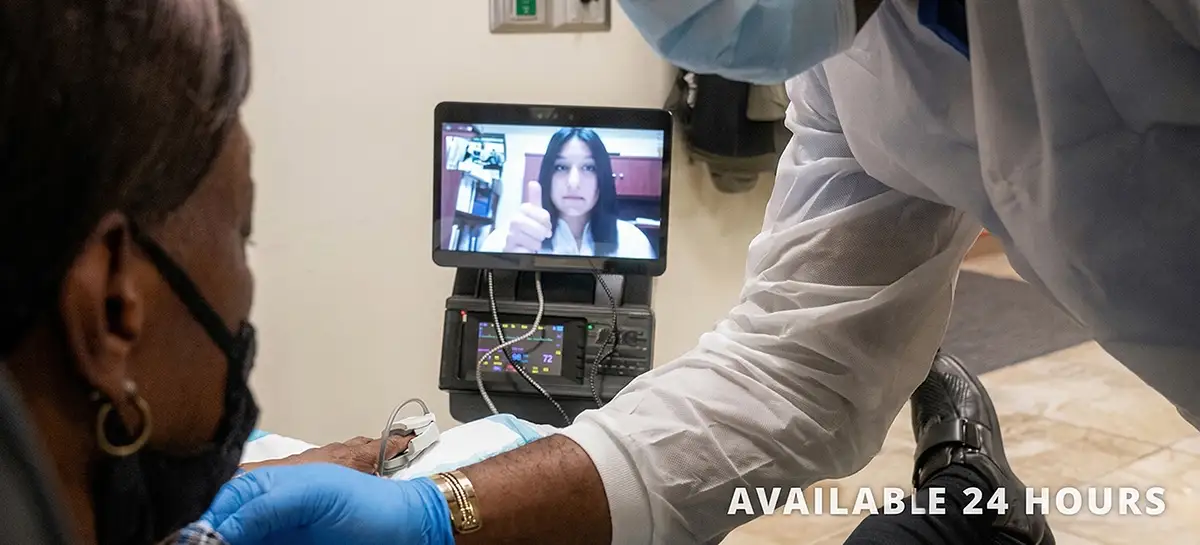
Continuous 24/7 tracking of patient vital signs at home or in the ICU via sensors.
Mobile medical robots in hospitals that facilitate real-time consultation, examination, and data transmission.
Telemedicine Investment ROI Analysis: Numbers Executives Need to Know
Any hospital investment decision must be based on measurable numbers. Here is the ROI analysis framework for Telemedicine investment used by hospital executives globally.

Costs Hospitals Can Reduce with Telemedicine
| Cost Category | Average % Reduced | Reduction Mechanism | Impact Level |
|---|---|---|---|
| Personnel Costs (Labor) | 20–35% | Robots replacing routine work / Increased productivity per headcount | Very High |
| Energy Costs | 15–25% | Reduced active OPD space / Lower foot traffic | High |
| Readmission Treatment Costs | 30–38% | Continuous remote monitoring of chronic patients at home | Very High |
| Document Management Costs | 40–60% | Automated EMR connected to Telemedicine | Medium |
| Hospital Space Costs | 10–20% | Virtual OPD reduces the need for examination rooms | Long-term |
| PPE & Infection Control | 25–45% | Reduced physical contact between staff and patients | High |
Reducing Hospital Costs: How Can Telemedicine Save Energy?
One aspect hospital executives often overlook is energy costs, which account for 8–15% of total operating costs. Large hospitals with 500+ beds can have electricity bills as high as 30–80 million baht per year. Integrating Telemedicine impacts energy reduction in 3 main dimensions:
Reducing Foot Traffic in OPD: Patients using Virtual Clinics do not need to travel to the hospital, reducing electricity usage in examination rooms, waiting areas, and central air conditioning systems. It is estimated to reduce HVAC load by 12–18% in outpatient areas.
Robots Use Less Energy Than Staff: Robots like the temi V3 use only 100–240V and can automatically self-charge. Compared to the hidden energy costs of 1 employee (electricity, AC, office space), the savings are highly tangible.
Reducing the Number of Active Buildings: Remote consultations allow hospitals to minimize opening branch clinics or adjust operating hours in certain areas, resulting in a 15–25% reduction in total energy costs in the medium term.

5 Steps to Implement Telemedicine in Large Hospitals for Maximum ROI
Needs Assessment & Gap Analysis: Assess bottlenecks in the current patient care process. Analyze which departments have high routine workloads (OPD, IPD chronic follow-ups, ICU) and would benefit most from Telemedicine.
Choose a Telemedicine Solution that Supports Integration: The system must connect with the existing HIS (Hospital Information System), EMR/EHR, and HL7/FHIR standards, as well as support SDKs for developing hospital-specific applications.
3–6 Month Pilot Project: Start with 1–2 pilot departments. Set clear, measurable KPIs such as the number of patients served per day, average wait times, patient satisfaction, and cost per visit.
Staff Training and Change Management: The success of Telemedicine depends on staff adoption. Invest in training, create champions in each department, and communicate the expected ROI to the team.
Scale & Optimize: Once the pilot is successful, scale it hospital-wide. Measure actual ROI against the established baseline and continuously improve (Continuous Improvement).
ROI Comparison Table: Hospitals With vs. Without Telemedicine
| Metric | Standard Hospital (No Telemedicine) | Hospital Using Telemedicine | Difference |
|---|---|---|---|
| Cost per Visit (OPD) | 800–1,200 THB | 200–450 THB | Reduced by 60–70% |
| Average Wait Time | 45–90 Minutes | 5–15 Minutes | Reduced by 75–80% |
| Readmission Rate (30 Days) | 18–25% | 11–15% | Reduced by 38–42% |
| Patient Satisfaction (CSAT) | 3.4 / 5.0 | 4.3 / 5.0 | +26% |
| Revenue per Doctor/Day | 20–30 Visit | 45–80 Visit | +150–170% |
| Annual Energy Costs | 100% | 75–85% | Reduced by 15–25% |

Things Hospital Executives Should Evaluate Before Investing in Telemedicine
- Daily OPD patient volume and the proportion of chronic disease patients who do not need physical exams at every visit
- Readmission costs, which are often hidden in the budget and unmeasured
- Energy and space expenses paid for underutilized areas
- Potential to generate new revenue from Virtual Consultations, both domestic and international
- Ability to connect with existing IT systems (Legacy System Integration)
- Thai Ministry of Public Health regulations related to Telemedicine
temi V3 — Smart Telemedicine Robot for Large Hospitals
An AI robot that allows doctors to consult patients from anywhere via high-definition video calls. It navigates autonomously in hospitals, supports SDKs to connect with HIS/EMR systems, and operates for 8 continuous hours per charge. Includes an ROI Calculator to estimate returns before making a decision.

Use Cases: How Does Telemedicine Practically Reduce Hospital Costs?
Use Case 1: ICU Telemedicine (Tele-ICU)
Hospitals in the US using Tele-ICU systems reduced ICU mortality rates by 20% and ICU costs by an average of $3,000–$5,000 per patient, as one intensivist can monitor multiple ICU branches simultaneously via Remote Monitoring.
Use Case 2: Virtual OPD for Chronic Patients
Managing diabetes, hypertension, and heart disease through Telemedicine helps hospitals reduce the cost per visit by 60–70% compared to in-person appointments, while patients still receive close monitoring.
Use Case 3: Telemedicine Robots in Wards
Hospitals using Telemedicine robots in patient wards can reduce direct physical contact between staff and contagious patients by 40–60%. This significantly lowers PPE costs and Hospital-Acquired Infection (HAI) rates, which have an average cost of 40,000–80,000 THB per case.
FAQ
Telemedicine refers specifically to providing clinical services via remote technology (e.g., diagnosis, prescribing medication, treatment). Telehealth is broader, encompassing Telemedicine plus non-clinical health services like health education, personal health management, and staff training.
Large hospitals systematically implementing Telemedicine generally see an average ROI of 150–300% within 3 years. This comes from reducing personnel costs by 20–35%, energy costs by 15–25%, readmission rates by 30–38%, and increasing revenue from Virtual Visits unconstrained by physical locations.
Telemedicine investment costs for large hospitals fall into 3 tiers:
(1) Basic system (Video Platform + Software) approx. 500k–2M THB/year
(2) Mid-tier (Platform + Remote Monitoring) approx. 2–8M THB/year
(3) Comprehensive system with Telemedicine robots approx. 8–30M THB. The payback period is usually 12–24 months
Thailand has established Telemedicine guidelines via the Ministry of Public Health under the government's Digital Health policy. Doctors are allowed to provide digital consultations under specific conditions, including securing patient data (PDPA Compliant) and proper identity verification standards. Hospitals should consult specialized legal advisors before implementation.
Telemedicine robots are suitable for hospitals with high patient volumes and large spaces. Specifically: Regional centers and large general hospitals (200+ beds), hospitals with multiple ICUs, hospitals with infectious disease wards, and hospitals wanting to provide cross-departmental Specialist Consultations. Robots like the temi V3 support SDKs, allowing flexible integration with existing HIS and EMR systems.
Request a Demo
Please provide your complete information.



















